A Case for Cleaner Air
Credit: Adam Squires, Biophysical Chemist, Bath University lead www.aerosol-cdt.ac.uk
Airborne respiratory diseases (TB, Covid etc) are all transmitted the same way: pathogen is in tiny particles that we breathe/cough/speak out. They’re small enough to stay in the air like smoke, you get more if you’re closer but eventually, the whole room is smoky. People breathe them in, and get infected. More particles are given out through talking, shouting or singing. Because the virus is in these same particles, it doesn’t matter what variant of covid it is.
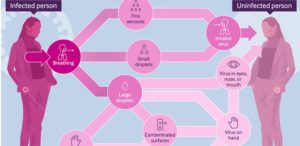 Check the above risk calculator at https://www.bmj.com/content/375/bmj-2021-065312
Check the above risk calculator at https://www.bmj.com/content/375/bmj-2021-065312
Masks?
If we can stop people breathing in respiratory particles from someone who’s infected, we can stop airborne diseases from spreading. There are 4 ways to do this: masks; fresh air (ventilation); filtering (HEPA); and sterilising the air (UV). Masks are good. Blue (“surgical”) > cloth > nothing. Mainly stop wearer unwittingly infecting others, so good if everyone wears them. (Stops particles in a jet from mouth/nose). Well-fitting FFP2 / FFP3 even better, protect wearer too; can be reworn. However, masks, while important, are not enough for long periods of time in the same room (like in schools or offices) and can’t be worn when eating and drinking. Plus there are no masks in UK primary schools and they’re not a (nice) long-term solution. This is often where the confusion lies. The difference in masks being useful in passing another person briefly compared to masks being useful with extended exposure.
Ventilation
2nd option, flush the old exhaled particle-filled air out with fresh air (“ventilation”) – mechanically through building ductwork, or naturally by opening a window. Window ventilation depends on weather & can be hard to judge. To know if need more fresh air, we use CO2 to estimate the number of respiratory particles built up in the air (hard to measure) – we breathe both out, and they’re both removed by ventilation. Outdoor fresh air is 400 ppm CO2 (global warming!). Above 800 ppm, >1% of the air in the room has been breathed out, so you want to get fresh air in by opening windows. Quick blast to refresh if too cold to leave open.

If the weather has a breeze, opening windows on both sides of the building (with internal doors open) can help to get a flow of air across the space. If it’s cold keeping windows open for long periods, opening them wide for a few minutes every hour can allow enough air through to take away possible virus in the air with less effect on comfort. If you have mechanical ventilation in the building (many newer buildings should) check whoever manages your building: have set it to maximise fresh air (not “recycled” as per our blog early 2020). Can check all OK with CO2 monitor too. If you can’t get enough fresh air (can’t open the windows enough / too cold) so CO2 usually > 1200ppm by end of a school lesson for example: you can also *filter out* the infectious aerosols from the air.
HEPA
Do this with HEPA (“high efficiency particulate air [filter]”Many home “air purifiers” are HEPA. They’re plug-in portable boxes the size of a bin, that suck air in the sides & blow filtered air out the top. You need 2 or 3 to a classroom or office depending on room size, dotted around (see later). [NB they don’t remove CO2 so CO2 monitors won’t show the HEPA benefit] HEPA is a well-established technology, that removes all particles in the 0.1-10 micron size range, which includes the exhaled particles carrying airborne diseases (also pollen, smoke, particulate pollution etc).
“H13 HEPA” removes 99.95% of the particles. ultraviolet light kills virus in airborne particles: in sunlight, or units fitted indoors (widely used for measles and tuberculosis) https://www.cibsejournal.com/technical/leading-light-ensuring-effective-use-of-uv-technology-in-buildings/ Needs specialist fitting and high ceilings (for safety) but is good for large rooms (canteens, gyms) With high covid rates, you want clean air *and* masks. When face to face unmasked, ventilation / HEPA / UV won’t stop infection: if you’re opposite a smoker, an open window won’t help too much if they’re breathing smoke into your face. Masks (esp.FFP2) provide that protection. Fresh, clean or sterilised air is extremely good at reducing transmission and works on *any* variant, and other airborne infectious diseases too. It’s a good long-term investment, and it’s also *very do-able*.
CDL Products
Cool Designs are currently working with Carrier Air Conditioning and we stock the following:

Carrier CAFN026LC2 suitable for up to 210m3
Carrier CAFN036LC2 suitable for up to 410m3
Carrier CAFN051LC2 suitable for up to 610m3
These small portable air purifiers have HEPA 13 filters and UV-C filtration (see datasheet links above)
A step up from this is the Carrier Opticlean.
The OptiClean rolls easily into any room and plugs into a standard electrical outlet to quickly improve indoor air quality (IAQ) in schools, dental offices, hospitals, and other commercial facilities. It can be operated in two modes: 
Air Scrubber—uses 99.97% efficient, long-life HEPA filters to remove particles as small as 0.3 microns, then discharge cleaner air back into the room. Ideal for a wide range of commercial applications, including K–12 classrooms, dental office exam rooms and open-air, temporary medical facilities.
Negative Air Machine—helps convert normal hospital rooms into negative-pressure airborne infectious isolation rooms (AIIR) by adding a vacuum effect to the HEPA filtration capability. Designed to ASHRAE Standard 170 for Ventilation of Health Care Facilities.
The units can be operated either vertically or horizontally in both modes.
OptiClean YouTube video: https://www.youtube.com/watch?v=bLlKTGztUkY&t=1s
Caveat: clean air is an extra layer. Face to face unmasked = still high risk (esp indoors). Distancing also helps (as with smoker analogy). And without distancing or masks, clean air may still make difference, eg infecting only 1 or 2 classmates/office workers, not 10. But not a magic bullet. School study from elementary schools in Georgia. 48% lower incidence from combined ventilation + HEPA. 31% reduction from HEPA alone. These are lower estimates from the effect on *in classroom* infections because students can get infected out of class
Further Research
When a team of doctors, scientists and engineers at Addenbrooke’s Hospital and the University of Cambridge placed an air filtration machine in COVID-19 wards, they found that it removed almost all traces of airborne SARS-CoV-2. A team at the University of Cambridge and Cambridge University Hospitals (CUH) NHS Foundation Trust investigated whether portable air filtration/UV sterilisation devices could reduce airborne SARS- CoV-2 in general wards that had been repurposed as a COVID ward and a COVID Intensive Care Unit (ICU). The results are published in Clinical Infectious Diseases.
Full article: https://www.cam.ac.uk/research/news/air-filter-significantly-reduces-presence-of-airborne-sars-cov-2-in-covid-19-wards
Reference
Conway Morris, A, et al. The removal of airborne SARS-CoV-2 and other microbial bioaerosols by air filtration on COVID-19 surge units. Clin Inf Dis; 30 Oct 2021; DOI: 10.1093/cid/ciab933